Advancing Healthcare Excellence Through Technology

Where Service Meets Compassionate Care
At Cuttlesoft, we combine cutting-edge technology with deep healthcare insights to develop software that truly enhances healthcare operations.
By simplifying complex processes and improving system efficiency, our process allows your team to focus on delivering excellent care.
Our Advantage
Industry Expertise
User-Centric Design
Compliance Focused
Proactive Support and Maintenance
Customized Solutions
Cuttlesoft understands that no two healthcare organizations are the same. Whether it's managing patient records more efficiently, streamlining appointment systems, or enhancing telehealth offerings, we've got you covered.
Regulatory Compliance
Ensure full compliance with healthcare laws and standards with software designed for peace of mind. Cuttlesoft has the expertise to navigate the complex landscape of healthcare regulations, including HIPAA, HITECH, and GDPR.
Scalable Architecture
We build systems designed to expand effortlessly as your patient or client load increases and healthcare technologies evolve. Scaling means you can adapt to future healthcare challenges without the need for constant system overhauls.
Featured Case Study
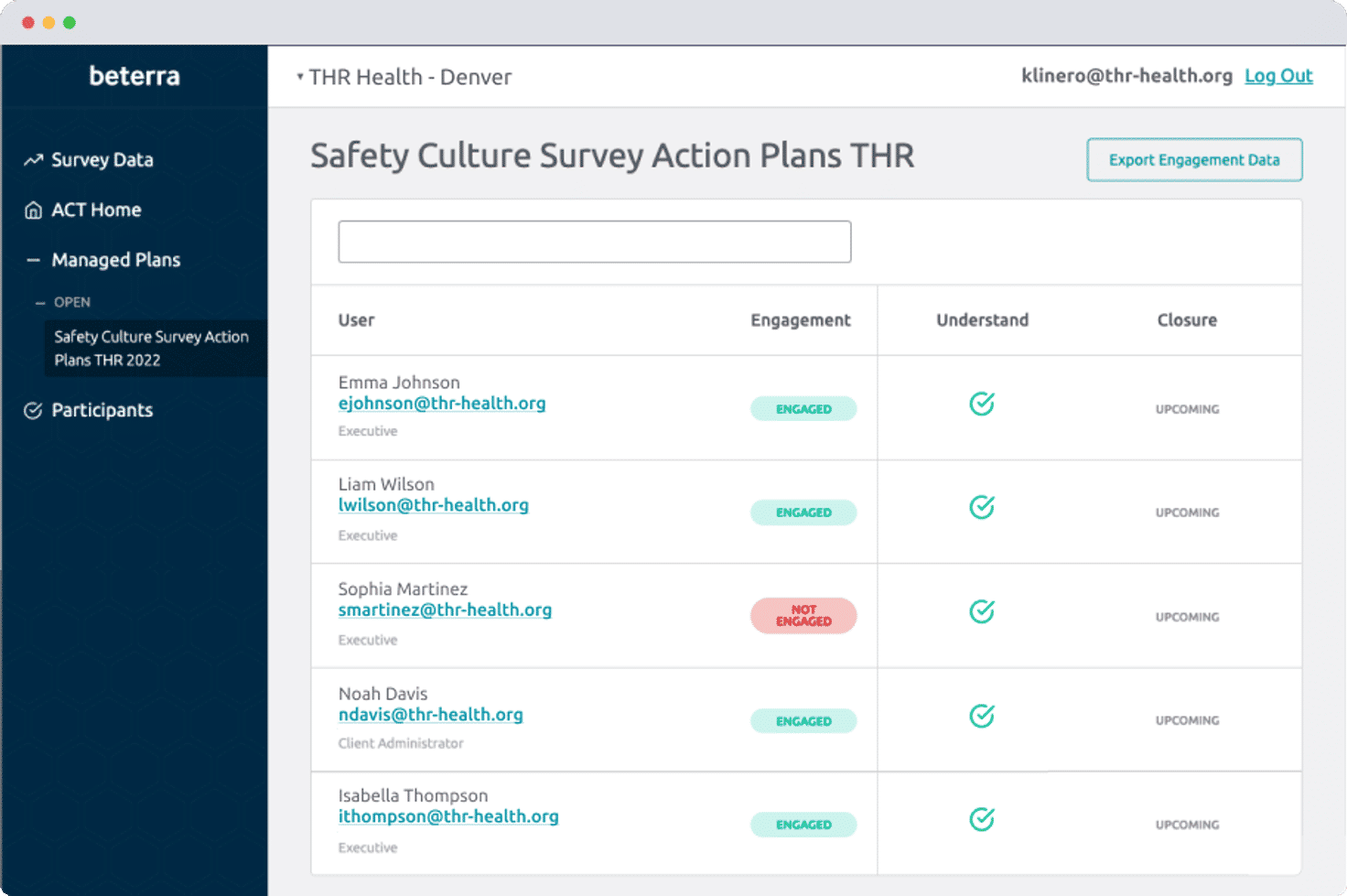
Beterra HealthHow Cuttlesoft helps Bettera Health improve engagement, safety, and patient care with data-driven technology.
Read MoreTrusted by these and other amazing partners







Advanced Security Measures
Safeguarding patient data and ensuring compliance are at the core of our development process. We implement robust security protocols and adhere to strict compliance standards to maintain the highest levels of data confidentiality and integrity.
- HIPAA
- HITECH
- GDPR
- CCPA


Seamless Integration
Cuttlesoft is committed to enhancing your healthcare operations through seamless integration of new software with your existing systems. We focus on creating interfaces that promote efficient workflows, allowing your team to adopt new functionalities without a steep learning curve.
- HL7 FHIR
- EMR Integrations
- Epic: App Orchard
Healthcare Software Development FAQs
HIPAA compliance is built into our development process from day one, not added as a checklist at the end. We implement the technical safeguards required by the HIPAA Security Rule: AES-256 encryption for data at rest, TLS 1.2+ for data in transit, role-based access control (RBAC) so users only see the Protected Health Information relevant to their role, and comprehensive audit logging that tracks every access event for compliance reporting. We also implement automatic session timeouts, multi-factor authentication, and IP-based access restrictions where appropriate. On the operational side, Cuttlesoft signs Business Associate Agreements (BAAs) with our healthcare clients and maintains our own internal security policies aligned with HIPAA administrative safeguards. We conduct risk assessments at the start of every healthcare engagement to identify vulnerabilities specific to that project's architecture. Our infrastructure runs on HIPAA-eligible services from AWS and GCP, both of which provide BAA coverage for their compliant service tiers.
We build custom healthcare applications across the full care delivery spectrum. Our work includes patient-facing mobile apps (appointment scheduling, telehealth, remote patient monitoring, medication adherence), provider-facing tools (clinical dashboards, care coordination platforms, electronic health record extensions), and operational systems (revenue cycle management integrations, analytics dashboards, HIPAA-compliant data pipelines). We have built digital therapeutics applications that are clinically validated, including Easeday, a mobile app clinically proven to reduce migraine frequency that we developed in React Native. We have also worked with Beterra Health to build data-driven tools that improve patient engagement and safety outcomes. Whether you need a standalone mobile health app or a system that integrates with existing clinical infrastructure, our team has the healthcare domain experience to build it right.
Interoperability is one of the most technically challenging parts of healthcare software development, and it is a core competency for our team. We implement HL7 FHIR (Fast Healthcare Interoperability Resources) as the primary standard for data exchange. FHIR uses RESTful APIs and standardized resource types (Patient, Observation, MedicationRequest, Encounter, and others) to enable structured data sharing between systems. For EHR integration specifically, we work with Epic's App Orchard and similar marketplace programs that require SMART on FHIR authentication, which handles OAuth 2.0-based authorization so that third-party apps can securely access patient data within the EHR context. When clients need to connect to legacy systems that use older HL7 v2 messaging or proprietary interfaces, we build translation layers that map between formats while preserving data integrity. We also implement IHE (Integrating the Healthcare Enterprise) profiles where needed, particularly for clinical document exchange using CDA (Clinical Document Architecture) standards.
Yes. EHR integration is a standard part of our healthcare development work. The approach depends on your EHR vendor and what level of access you need. For Epic environments, we build SMART on FHIR apps that can be launched directly from within the EHR, accessing patient context and clinical data through Epic's FHIR R4 APIs. This path requires App Orchard certification, which involves security review, data use attestation, and testing against Epic's sandbox environments. We guide clients through that process. For other EHR platforms, we work with whatever integration interfaces are available: FHIR APIs, HL7 v2 messaging, direct database access where permitted, or middleware platforms like Mirth Connect or Redox that normalize data exchange across vendors. The goal is always to build integrations that work within your existing clinical workflow rather than forcing your staff to switch between systems. We design interfaces that surface relevant data at the point of care, so clinicians do not need to leave the tools they already use.
Our healthcare technology stack is chosen for security, reliability, and long-term maintainability. For backend systems, we primarily build with Python and Django, which provides a mature ORM, built-in authentication framework, and a strong ecosystem of security-focused libraries. Django's middleware architecture makes it straightforward to implement audit logging, request validation, and encryption at the application layer. For patient-facing mobile applications, we build with React Native and Expo, which lets us ship cross-platform iOS and Android apps from a single codebase while still accessing native device APIs like HealthKit, Google Fit, biometric sensors, and push notifications. For data-intensive healthcare applications that require real-time dashboards or analytics, we use React on the frontend with PostgreSQL databases and, where needed, cloud services from AWS or GCP that are covered under HIPAA BAAs.
Legacy system migration in healthcare carries higher stakes than in most industries because downtime can affect patient care and data loss can create compliance violations. We approach migrations incrementally rather than as a single cutover. The typical process starts with a thorough audit of the legacy system: its data model, integrations, business logic, and any undocumented workflows that staff rely on. We then build the replacement system in parallel and implement data migration pipelines that map legacy schemas to the new structure, validate data integrity at every step, and preserve complete audit trails as required by HIPAA. We run dual systems during a transition period so clinical operations continue uninterrupted. Once the new system is validated and staff are trained, we coordinate the cutover with minimal downtime, typically during off-peak hours. Historical data, including patient records, encounter histories, and billing data, is migrated and verified before the legacy system is decommissioned. We have done this for clients moving off aging platforms where vendor support had ended, and the pattern is always the same: no data loss, no workflow disruption, no compliance gaps.
Healthcare projects generally take longer than comparable non-healthcare applications because of compliance requirements, integration complexity, and the testing rigor that patient-facing software demands. A focused mobile health app (patient portal, appointment scheduling, telehealth interface) typically takes three to five months. A more complex system involving EHR integration, custom clinical workflows, and multi-role access control usually takes five to nine months. Large-scale platforms with multiple integration points, analytics, and regulatory certification requirements can take nine months or longer, often delivered in phased releases. These timelines include discovery, architecture, development, testing, compliance validation, and deployment. The single biggest variable is integration scope. A standalone HIPAA-compliant app is straightforward. An app that needs to exchange data with Epic, process HL7 messages, and connect to a claims clearinghouse requires significantly more architecture and testing time. We scope every healthcare project individually and provide a detailed timeline after the discovery phase. Learn more about how we structure engagements.
We implement defense-in-depth security, meaning multiple layers of protection so that no single point of failure exposes patient data. At the infrastructure level, we deploy on HIPAA-eligible cloud services with encrypted storage volumes, isolated VPCs, and network access control lists. At the application level, we implement field-level encryption for PHI, so sensitive data like Social Security numbers, diagnoses, and medication lists are encrypted individually within the database, not just at the disk level. Access control follows the principle of least privilege: every user role is scoped to the minimum data needed for their function, and every access event is logged to an immutable audit trail. We conduct security testing throughout development, including automated static analysis, dependency vulnerability scanning, and manual penetration testing before launch. Post-deployment, we monitor for anomalous access patterns and maintain an incident response plan that meets the HIPAA Breach Notification Rule's requirements for identifying, containing, and reporting any security incidents within the required timeframes.
Yes. Healthcare applications require more active maintenance than typical software because the regulatory and technical landscape shifts constantly. Apple and Google release major OS updates annually that can affect HealthKit or Google Fit integrations, HIPAA guidance evolves, EHR vendors update their APIs, and security vulnerabilities in dependencies need to be patched promptly. Our maintenance engagements for healthcare clients cover dependency updates and security patching, HIPAA compliance monitoring and documentation updates, EHR and third-party API version upgrades, App Store and Play Store submission management (including privacy manifest updates on iOS), performance monitoring and incident response, and feature enhancements as clinical workflows evolve. We also handle the compliance documentation side: maintaining up-to-date risk assessments, audit logs, and BAA documentation as your system changes over time. Maintenance is not optional for healthcare software. A HIPAA-compliant app that falls behind on security patches is a liability. Contact us to discuss a support plan for your healthcare application.